Researchers at the University’s Scalp Cooling Research Centre have discovered the world’s first piece of biological evidence that explains how scalp cooling actually works and the mechanism behind its protection of the hair follicle
GROUND-BREAKING research from the University of Huddersfield, announced in celebration of World Cancer Day 2021, proves that scalp cooling physically protects hair follicles from chemotherapy drugs. It is the world’s first piece of biological evidence that explains how scalp cooling actually works and the mechanism behind its protection of the hair follicle.
The study, entitled ‘Cooling-mediated protection from chemotherapy drug-induced cytotoxicity in human keratinocytes by inhibition of cellular drug uptake’, has been published in the peer-reviewed journal PLOS ONE.
The data was part of an innovative hair follicle research project carried out by the dedicated Scalp Cooling Research Centre based at the University of Huddersfield. It involved the cultivation of cells isolated from human hair follicles in the lab.
“We were able to measure how much chemotherapy drug goes into the cultured cells from hair follicles and what we have found is cooling actually dramatically reduces the amount of chemotherapy drug being absorbed by the rapidly-diving cells of the hair follicle.”
Dr Nik Georgopoulos
The £1 million research centre was established at the University in 2019 with the backing of Huddersfield firm Paxman – global leaders in scalp cooling technology.
The team of experts from biology and design technology have been working together with the aim of Paxman becoming the only hair loss-preventing scalp cooling provider firmly based on biological research. It also brings the family-run business one step closer to achieving its vision of ‘zero hair loss’ for cancer patients undergoing chemotherapy treatment.
Chemotherapy works by targeting all rapidly dividing cells in the body. Hair is the second fastest dividing cell, and this is the reason why many chemotherapy drugs cause alopecia. The hair follicles in the growth phase are attacked, resulting in hair loss approximately two weeks after the commencement of chemotherapy treatment.
Co-director of the centre and lead author of the journal article is Dr Nik Georgopoulos, a cancer expert at the University’s Department of Geographical and Biological Sciences who has collaborated with Paxman since 2011.
“Scalp cooling is currently the only treatment to combat ‘chemotherapy-induced alopecia’, yet little is known about its cytoprotective effect on human hair follicles,” said Dr Georgopoulos, who talks about the science behind scalp cooling with his University colleague Dr Andrew Collett in the video below.
Before now, he explained, the most common and obvious presumption to describe how scalp cooling worked was that as the scalp is cooled, the veins become constricted thereby reducing the amount of blood flow, meaning less of the chemotherapy drug enters the hair follicle.
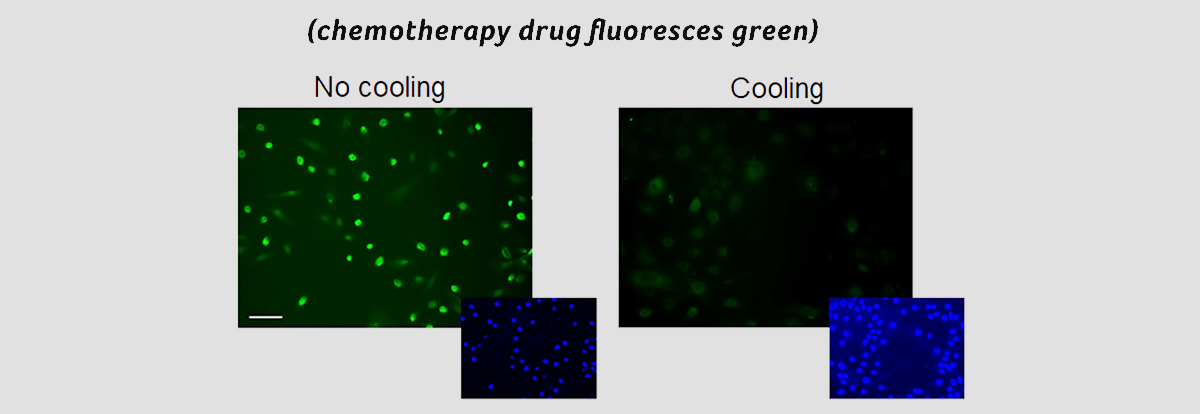
“However, this is a really exciting discovery because our research now shows it is not as simple as that. We were able to measure how much chemotherapy drug goes into the cultured cells from hair follicles and what we have found is that cooling actually dramatically reduces the amount of chemotherapy drug being absorbed by the rapidly-diving cells of the hair follicle,” he added.
This means there is now evidence for the first time, which demonstrates cooling has a direct effect on reducing the amount of drug that goes in and not an indirect effect as thought before with the restricted blood flow.
“Our results provide evidence that attenuation of cellular drug uptake represents at least one of the mechanisms underpinning the ability of cooling to rescue human keratinocytes from chemotherapy drug-cytotoxicity, thus supporting the clinical efficacy of scalp cooling,” he added.
The Centre has also been working on developing innovative scalp cooling related treatments and individual 3D-printed cooling caps. This has involved a collaboration of researchers from across two of the University’s schools of study, Applied Sciences and Art, Design and Architecture.
“This latest project builds upon our previous research,” continued Dr Georgopoulos.
“We had already demonstrated that if you cool at just 3 or 4 degrees lower, this can be the difference between the cells surviving or dying. We have now shown that a few degrees in temperature can also mean a more dramatic reduction in chemotherapy drug uptake by cells.
“The more evidence we can provide, the more data the designers have to facilitate the design of a better a cap. A better fit could mean more of a reduction in temperature, so more effective cooling means more survival of the follicles, leading to a better outcome.”
The percentage of hair loss can be further reduced when scalp cooling is combined with the application of a topical agent. One of the Centre’s tasks has been to develop the best way to deliver this agent to hair follicles on the scalp.
Richard Paxman, CEO of Paxman, added: “This latest research brings us one step closer to achieving our vision of ‘zero hair loss’ for cancer patients undergoing chemotherapy treatment. This is fabulous news and is a ground-breaking step in the field of scalp cooling research.”
Latest news from the Department of Biological and Geographical Sciences
Latest news from the Department of Biological and Geographical Sciences - 0 articles matching your search
Latest news from the Department of Biological and Geographical Sciences - 1 article matching your search
Latest news from the Department of Biological and Geographical Sciences - {{numberOfPosts}} articles matching your search
